
ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 1
Electronic Health Record Adoption and Interoperability among U.S.
Skilled Nursing Facilities and Home Health Agencies in 2017
JaWanna Henry, MPH; Yuriy Pylypchuk, PhD; Vaishali Patel, PhD MPH
Interoperability has the potential to improve transitions of care between acute-care and post-acute care facilities; such as
skilled nursing facilities (SNFs) and home health agencies (HHAs) (1). Poor communication and coordination during these
transitions may lead to adverse events including readmissions and medication errors. Federal policies aim to advance
interoperability in post-acute care settings. The Improving Medicare Post-Acute Care Transformation Act (IMPACT Act) of
2014, for example, requires assessment data to be standardized and interoperable to allow for the exchange of data
among post-acute care providers and other providers (2,3). This brief describes the state of health IT use among HHAs
and SNFs in 2017. Specifically, it presents key measures on electronic health record (EHR) adoption and interoperability
from nationally representative surveys of SNFs and HHAs. The data brief also describes variation in interoperability by
method of electronic exchange and examines the extent to which these facilities have information electronically available
at the point of care. Finally, this data brief reports on the use of mobile and telehealth technologies among HHAs.
HIGHLIGHTS
4 More HHAs (78 percent) adopted EHRs than SNFs (66 percent) in 2017.
4 The ability to integrate patient health information received from outside facilities lagged behind for both HHAs
(36 percent) and SNFs (18 percent) compared to these facilities’ engagement in other domains of
interoperability.
4 HHAs (32 percent) and SNFs (37 percent) most commonly used their EHR to exchange health information.
4 HHAs and SNFs that use three methods of exchange are more likely to have information electronically available.
4 Nearly 40 percent of HHAs used telehealth technology to keep track of patients’ health between in-person visits.
EHR adoption rates were higher among HHAs compared to SNFs.
Figure 1: Percent of HHA and SNFs that used an EHR, 2017.
SOURCE: 2017 IQVIA Nursing Home, n=1,000 and 2017 IQVIA Home Health Agency, n=1,004. See Definitions for EHR description.
Notes: * Difference is statistically significant at p<0.05.
« In 2017, over three-quarters of HHAs and two-thirds of SNFs reported they had adopted EHRs.
EHR
78%*
No EHR
22%
HHA
EHR
66%
No EHR
34%
SNF

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 2
Among facilities with an EHR, a majority of HHAs and SNFs used their EHR for medication
management purposes.
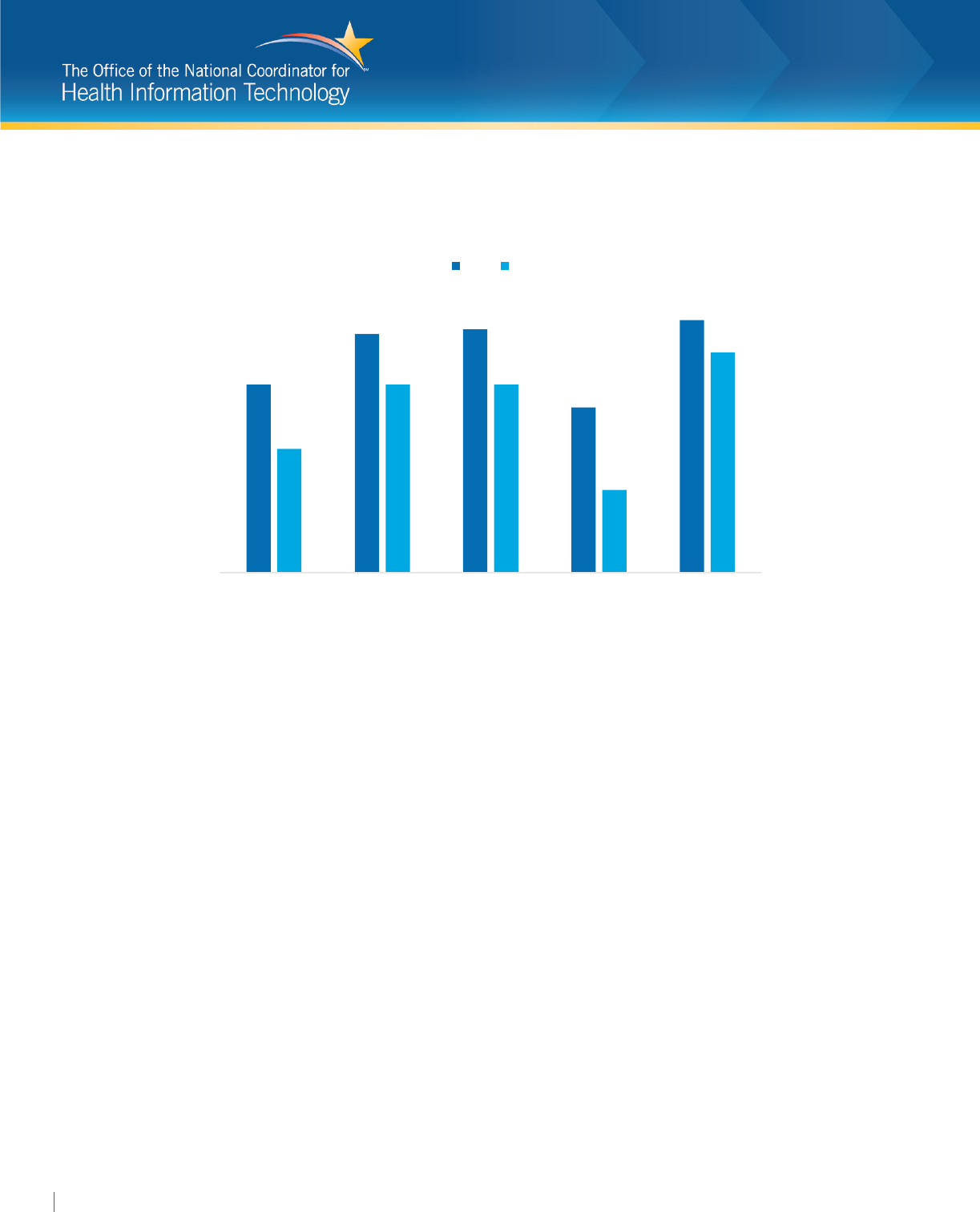
Figure 2: Percent of SNFs and HHAs with an EHR that used medication management functions, 2017.
SOURCE: 2017 IQVIA Nursing Home, n=1,000 and 2017 IQVIA Home Health Agency, n=1,004.
Notes: * Difference is statistically significant at p<0.05. The denominator includes HHAs and SNFs that adopted an EHR.
« HHAs had higher rates of recording and reconciling patient medications using an EHR compared to SNFs.
« Almost all HHAs used their EHRs to record patient medications and reconcile medications.
« Almost 9 out of 10 SNFs with an EHR recorded patient medications using an EHR.
99%*
98%*
87%
83%
Record Patient Meds
Reconcile Patient Meds
SNF HHA
ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 3
HHAs are more likely than SNFs to engage in each domain of interoperability.
Figure 3: Percent of SNFs and HHAs with an EHR that reported having the ability to electronically send, receive, find, and
integrate patient health information, and have outside information available, 2017.
SOURCE: 2017 IQVIA Nursing Home, n=1,000 and 2017 IQVIA Home Health Agency, n=1,004 Census.
Notes: * Difference is statistically significant at p<0.05.
« About half of HHAs engaged in electronically sending or receiving patient health information from outside
providers; compared to four out of 10 SNFs.
« Integration of received information lagged behind other interoperability domains for both HHAs and SNFs.
« More HHAs (41 percent) had the ability to find patient’s health information from outside facilities than SNFs (27
percent).
« HHAs were twice as likely to integrate patient health information than SNFs.
« Nearly half of HHAs (55 percent) and SNFs (48 percent) had information available from outside providers at the
point of care.
41%*
52%*
53%*
36%*
55%*
27%
41% 41%
18%
48%
Find Send Receive Integrate Outside Info
Available
HHA SNF

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 4
About one-third of HHAs and SNFs relied on EHRs alone to electronically exchange patient health
information.
Table 1: Percent of HHAs and SNFs that used different methods of electronic exchange (EHR alone, health information
organization (HIO), and read only access, 2017.
SOURCE: 2017 IQVIA Nursing Home, n=1,000 and 2017 IQVIA Home Health Agency, n=1,004.
Notes: *Difference is statistically significant between HHAs and SNFs at p<0.05. Read Only is defined as a permission to access files or directories where the user is
only allowed to read, not make changes.
« About 43 percent of HHAs and 29 percent of SNFs used more than one method for electronic exchange.
« Nearly one-third of SNFs did not use an EHR, HIO, or read-only access to an EHR for electronic exchange of
patient health information.
« A greater proportion of HHAs (20 percent) used all three methods of electronic exchange (EHR and HIO and
read-only access) than SNFs (eight percent).
« Nearly one-fifth of HHAs (19 percent) and SNFs (17 percent) exchanged data using an EHR and read-only access.
« Neither HHAs nor SNFs used both HIO and read-only access for electronic exchange.
Methods of Exchange
HHA
SNF
EHR alone
32%
37%
EHR and HIO and Read-only access
20%
8%*
EHR and Read only access
19%
17%*
No EHR, HIO, or Read-only access
23%
32%*
EHR and HIO
4%
4%
HIO alone
1%
1%
Read-only access alone
1%
1%
HIO and Read-only Access
0%
0%

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 5
SNFs that used EHRs, HIOs, and read-only access were twice as likely to have clinical information
from outside organizations electronically available than SNFs that only used an EHR.
Table 2: Interoperability domains (send, receive, find, integrate) by methods of exchange for HHAs and SNFs.
SOURCE: 2017 IQVIA Nursing Home, n=1,000 and 2017 IQVIA Home Health Agency, n=1,004.
« Among HHAs that use an EHR, HIO, and read-only access, almost all facilities (94 percent) had the ability to
query for patients’ health information from outside facilities.
« Using EHR, HIO, and read-only access enabled eight out 10 SNFs to routinely send and receive information with
outside organizations.
« HHAs using all three methods of electronic exchange had higher rates of reporting electronic availability of
patient health information at the point of care compared to those that used only an EHR.
Method used to exchange
Facility Type
Find/Query
Send
Receive
Integrate
Outside
Information
Available
EHR alone
HHA
19%
51%
50%
32%
62%
SNF
24%
44%
42%
18%
32%
EHR and Read-only Access
HHA
55%
67%
70%
58%
67%
SNF
51%
56%
56%
32%
41%
EHR and HIO and Read-only
Access
HHA
94%
76%
83%
60%
76%
SNF
74%
82%
81%
46%
68%

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 6
Almost three out of four HHAs used mobile technology during patient visits.
Figure 4: Use of mobile technology (e.g., laptops, tablets and smartphones) during patient visit.
SOURCE: 2017 IQVIA Home Health Agency, n=1,004.
Notes: Denominator of Mobile Technology Data Entry is among those who reported “Yes” to whether they use mobile technology.
« Among HHAs that use mobile technology during visits, most (85 percent) used devices to enter information
directly into their EHR system.
Yes 72%
No 26%
Do Not
Know 2%
Mobile Technology Use
Yes 85%
No 4.0%
Don't
Know 2%
NA 9.0%
Mobile Technology used to directly
enter data into EHR

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 7
About 4 out of 10 HHAs used telehealth technology to keep track of patients’ health between in-
person visits.
Figure 5: Rates of telehealth technology use among HHAs by ownership type and location (rural vs. urban).
SOURCE: 2017 IQVIA Home Health Agency, n=1,004.
Notes: Telehealth includes video conferencing or remote patient monitoring devices that collect data such as vital signs or blood sugar levels and transmit the data
back to the agency. *Difference is statistically significant at p<0.05.
« The use of telehealth technology does not vary by HHAs’ ownership status and location- almost 40 percent of
HHAs used telehealth for tracking patients’ health across each of these categories.
62%
61%
63%
63%
61%
38%
39%
37% 37%
39%
Overall Telehealth Government/
Non-profit
Private Urban Rural
No Yes

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 8
Summary
The nation’s aging population is projected to grow by 80 percent in the next 25 years (4). As a result, interoperability will
be important to ensure care coordination between acute care, post-acute care and other providers of care. A majority of
SNFs and HHAs have adopted EHRs. However, EHR adoption rates were higher among HHAs than SNFs. Among HHAs with
an EHR, a majority used their EHRs for both reconciling and recording medications. HHAs were also more likely to engage
in the use of these functions compared to SNFs.
HHAs and SNFs differed in their rates of engaging in the four interoperability domains: sending, receiving, finding, and
integrating health information received from outside sources. HHAs are more likely, than SNFs, to engage in each domain
of interoperability. Over half of HHA electronically sent or received health information; compared to 41 percent of SNFs.
However, both HHAs and SNFs had lower rates of electronically finding and integrating patient health data. Only 18
percent of SNFs report that they integrate patient health information electronically received from outside sources. Like
HHAs and SNFs, hospitals have a similar pattern related to interoperability; while a large proportion are electronically
sending and receiving health information fewer possess the capability to electronically find or integrate data from outside
sources.
Having patient health information electronically available from outside sources varied by the methods HHAs and SNFs
used to exchange information. An EHR was the most common method used to exchange information for both facility
types. Yet, at least 43 percent of HHAs and 29 percent of SNFs used more than one method for electronic exchange of
health information. Facilities that used multiple methods of electronic exchange, were more likely to engage in the four
interoperability domains. These facilities were also more likely to have information electronically available at the point of
care. For example, SNFs that use an EHR, HIO, and read-only access are twice as likely to have information available at
the point of care; compared to SNFs that use an EHR alone. Although using multiple methods increases the availability of
information, it also may increase the complexity and cost of of data exchange.
HHAs need to use technology during in home patient visits and to monitor patients between visits. Three-fourths of HHAs
(72 percent) used mobile technology. Among HHAs that used this technology, 85 percent used it during patient visits to
directly enter data into their EHR. About four in 10 HHAs (37 percent) used telehealth. There was no variation in the use
of telehealth technology by HHAs ownership status (private vs. not) or location (urban vs. rural).
Unlike hospitals and office-based physicians, SNFs and HHAs are not eligible to participate in the Medicare and Medicaid
Promoting Interoperability Programs, formerly known as the Medicare and Medicaid EHR Incentive Programs (5, 6).
However, implementation of federal policies, like the IMPACT Act, and the availability of interoperability standards for
standardized patient assessment data through resources such as the CMS Data Element Library
1
provide important
building blocks to advancing health information exchange. Policies that advance interoperability in the post-acute care
settings, are critical to ensuring that HHAs and SNFs are able to meet future demand for services and the complex health
needs of their patient population.
1
CMS Data Element Library (https://del.cms.gov/)

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 9
Definitions
Electronic Health Record (EHR): An Electronic Health Record (EHR) is an electronic version of a patient's medical history
that is maintained by the provider over time, and may include all of the key clinical data relevant to that person's care
under a particular provider, including demographics, progress notes, problems, medications, vital signs, past medical
history, immunizations, laboratory data and radiology reports.
Health Information Organization (HIO): A group of organizations within a specific geographic (state or regional) area that
share health care-related information, often via health information exchanges, according to accepted health care
information technology standards.
Interoperability: The ability of a system to exchange electronic health information with and use electronic health
information from other systems without special effort on the part of the user. This brief further specifies interoperability
as the ability for health systems to electronically send, receive, find, and integrate or use health information with other
electronic systems outside their organization.
Skilled Nursing Facility (SNF): Survey respondents that self-identified as a skilled nursing facility. Skilled nursing facilities
traditionally provide short-term, sub-acute care for persons recuperating from a hospitalization or an acute condition. See
Data Source and Methods section for more detail on sample of nursing homes.
Home Health Agency (HHA): Organizations that provide home-based healthcare services to patients with a medical illness,
chronic medical condition or a disability.
Mobile technology: tablets, smartphones, etc.

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 10
Data Source and Methods
The data presented in this brief are from the private company, IQVIA (formerly QuintilesIMS/ SK&A). IQVIA is a provider
of U.S. healthcare reference information including EHR adoption. In collaboration with ONC, IQVIA fielded a 10 question
telephone survey between September and November of 2017. Refer to the appendix for the subset of questions asked in
the survey and presented in this brief.
Over one thousand facilities rendering LTPAC services were surveyed. Of the facilities surveyed, 1,000 self-identified as a
SNF and 1,004 HHA.
Significant differences noted throughout the data brief were tested using p < 0.05 as the threshold.

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 11
References
1. Patel V., Pylypchuk Y., Henry J., & Searcy T. (July 2016) Variation in Interoperability among U.S. Non-federal
Acute Care Hospitals in 2015. ONC Data Brief, no.37. Office of the National Coordinator for Health Information
Technology: Washington DC.
2. IMPROVING MEDICARE POST-ACUTE CARE TRANSFORMATION ACT OF 2014 - IMPACT Act of 2014 - Public Law
113-185 - 113th Congress (2013-2014) https://www.congress.gov/bill/113th-congress/house-bill/4994/text.
3. IMPACT Act: Connecting Post-Acute Care across the Care Continuum. Centers for Medicare & Medicaid.
Available: https://www.cms.gov/Outreach-and-Education/Outreach/NPC/National-Provider-Calls-and-Events-
Items/2016-02-04-IMPACT-Act.html.
4. States Census. (2018) Older People Projected to Outnumber Children for First Time in U.S. History.
https://www.census.gov/newsroom/press-releases/2018/cb18-41-population-projections.html.
5. Office of the National Coordinator for Health Information Technology. 'Percent of Hospitals, By Type, that
Possess Certified Health IT,' Health IT Quick-Stat #52. dashboard.healthit.gov/quickstats/pages/certified-
electronic-health-record-technology-in-hospitals.php. May 2016.
6. Office of the National Coordinator for Health Information Technology. 'Office-based Physician Electronic Health
Record Adoption,' Health IT Quick-Stat #50. dashboard.healthit.gov/quickstats/pages/physician-ehr-adoption-
trends.php. December 2016.
Acknowledgements
The authors are with the Office of the National Coordinator for Health Information Technology (ONC). The data brief was
completed under the direction of Steve Posnack, Director of the Office of Technology and Talisha Searcy, Data Analysis
Branch Chief for the Office of Technology. Other staff that contributed to this document include Elizabeth Palena-Hall
from the Office of Policy at ONC.
Suggested Citation
Henry, J., Plypchuck, Y., & Patel, V. (November 2018) Electronic Health Record Adoption and Interoperability among U.S.
Skilled Nursing Facilities in 2017. ONC Data Brief, no. 41. Office of the National Coordinator for Health Information
Technology: Washington, DC.

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 12
Appendix
Appendix 1: Survey questions assessing EHR adoption and interoperability among skilled nursing facilities and home
health agencies.
Question Text
Response Options
SNF
Not including for accounting or billing purposes, does your facility currently use an
EHR to manage your patients' health records?
Yes | No | Don’t Know
HHA
Not including for accounting or billing purposes , does your home health agency
currently use an electronic health record to manage your patients' health records?
Yes | No | Don’t Know
SNF
Do staff at your skilled nursing facility electronically send key clinical information such
as labs, medications or problem lists to outside organizations on a routine basis?
Electronic does not include fax, e-fax or MDS (minimum data set) quality reporting.
Yes | No | Don’t Know
HHA
Does your agency electronically send key clinical information such as labs,
medications, or problem lists to outside organizations on a routine basis? Electronic
does not include fax, e-fax, or OASIS quality reporting.
Yes | No | Don’t Know
SNF
Do staff at your skilled nursing facility electronically receive key clinical information
such as labs medications or problem lists from outside organizations on a routine
basis? (Electronic does not include fax, e-fax or MDS (minimum data set) quality
reporting.
Yes | No | Don’t Know
HHA
Does your agency electronically receive key clinical information such as labs,
medications, or problem lists from outside organizations on a routine basis?
Electronic does not include fax, e-fax, or OASIS quality reporting
Yes | No | Don’t Know
SNF
Do staff at your skilled nursing facility electronically easily integrate patient health
information that you electronically receive into your EHR without manual entry or
scanning?
Yes | No | Don’t Know
HHA
Is the electronically received information easily incorporated or integrated into your
EHR without manual entry or scanning?
Yes | No | Don’t Know
SNF
Do staff at your skilled nursing facility electronically search or query for your patients'
health information from sources outside your facility? This might include through a
web portal, remote access to another facility or health information exchange
organization, for example.
Yes | No | Don’t Know
HHA
Does your staff electronically search or query for your patients’ health information
from facilities outside of your home health agency? This might include through a web
portal, remote access to another facility, health information exchange organization,
or through your EHR vendor’s network
Yes | No | Don’t Know
SNF
Does your skilled nursing facility use a state or regional health information exchange
organization (HIO) to electronically send, receive, integrate or search for patient
health information from outside sources?
Yes | No | Don’t Know
HHA
Does your home health agency use a regional, state or local health information
exchange organization (HIO) to electronically send, receive, or search for patient
health information from a variety of providers or other organizations outside your
organization? A Health Information Exchange Organization (HIO is a state, regional or
local organization that oversees and governs the electronic sharing of health-related
information among organizations. It does not refer to a private, closed network.
Yes | No | Don’t Know

ONC Data Brief ■ No. 41■ November 2018
ONC Data Brief No. 41|Electronic Health Record Adoption and Interoperability among U.S. Skilled Nursing Facilities and Home Health Agencies in 2017 13
SNF
When treating patients seen by other providers outside your skilled nursing facility,
how often does your staff have clinical information from outside encounters
electronically available at the point of care? Electronically available does not include
scanned or PDF documents. Is it often, sometimes, rarely or never?
Often | Sometimes |
Rarely | Never | Do Not
Know
HHA
When treating patients previously seen by other providers outside your home health
agency, how often do staff have clinical information from those outside encounters
electronically available at the point of care?
Often | Sometimes |
Rarely | Never | Do Not
Know
HHA
Do staff at your home health agency use an EHR system to record patients’
medications?
Yes | No | Don’t Know
SNF
Do staff at your skilled nursing facility use an EHR system to record patients’
medications?
Yes | No | Don’t Know
HHA
Do staff at your home health agency use an EHR system to reconcile medications?
Yes | No | Don’t Know
SNF
Does your skilled nursing facility use an EHR system to reconcile lists of patient
medications to identify the most accurate list?
Yes | No | Don’t Know
HHA
Do other facilities provide your home health agency with electronic, “read only”
access to their EHR systems? This means that your staff have the ability to view
patient health information in a third party’s EHR but not modify the record.
Yes | No | Don’t Know
SNF
Do external organization(s) provide your skilled nursing facility with electronic, “read
only” access to clinical information within their EHR systems? This means that
appropriate staff have the ability to view patient health information in a third party’s
EHR but not modify the record.
Yes | No | Don’t Know
HHA
Does your staff use telehealth technology to keep track of patients’ health (such as
vital signs, mobility or pain) between in-person visits? Telehealth includes video
conferencing or remote patient monitoring devices that collect data such as vital signs
or blood sugar levels and transmit the data back to the agency.
Yes | No | Don’t Know
HHA
Does your staff use mobile technology, such as laptops, tablets and smartphones,
during patient visits?
Yes | No | Don’t Know
HHA
Do staff directly enter information into your agency’s EHR system using mobile
technology (such as laptop, tablet or smartphone)?
Yes | No | Don’t Know
